DrCarney.com Blog
How Does Being Constipated Promote Varicose Veins?
Enlarged varicose veins are not only a cosmetic matter, they can cause aching pain, ulcers, burning, and cramping to varying degrees, and in some cases, more serious complications. The etiology of varicose veins can be multifactorial, says the scientific medical community — listing pregnancy, standing for long periods of time, a sedentary lifestyle, age, obesity, and family history as being the primary causes. However, the most significant contributing factor is repeatedly overlooked — the rich Western diet. Thanks to the dedicated work and observations made by Denis Burkitt, MD, (or "Fiber Man"), evidence revealing that a fiber-deficient diet is the major causative factor of many Western conditions, including varicose veins, hiatal hernia, hemorrhoids, colon polyps, and diverticulitis.
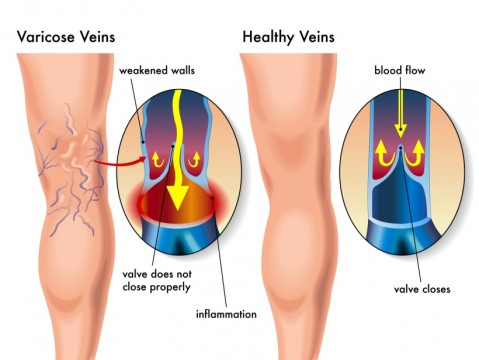
In order to understand how a fiber-deficient diet plays a role in developing varicose veins, keep in mind that when the heart pumps, it delivers oxygen-rich blood to the rest of the body via the arteries. The arteries then branch out into much smaller vessels, called capillaries, which deliver oxygen and nutrients to organs, tissues and cells. Blood depleted of oxygen is then returned back to the heart via the venous system. In order to keep the blood flowing in one direction (back to the heart), tiny one-way valves located throughout the veins prevents blood from flowing backward. These valves open as blood flows back to the heart and then close to stop the blood from becoming stagnant. Healthy valves keep the blood flowing freely back to the heart so that it can be recirculated. When the valves become weak or damaged, optimal blood flow is interrupted, and can back up and pool in the veins. Veins begin to bulge, and swell, and become distorted and tortuous (twisted) as venous pressure and congestion increases. Varicose veins are blue or purple due to the deoxygenated blood they contain as it travels back to the heart and lungs. The veins in the legs are most commonly affected due to the blood having to work against gravity to push the blood "uphill" in order to return to the heart. Dr. John McDougall explains this by saying that the distance from our feet to our heart is about four to five feet when we are standing, therefore, "A column of blood this tall would place tremendous pressures due to the weight of the blood on the veins in the lower leg and feet."
As we walk, muscles in the legs assist blood flow back to the heart by contracting and acting as pumps. The elasticity of the vein walls also facilitates blood to return to the heart. Since veins close to the surface of the skin have less muscle support than deep veins, these are the most afflicted.
One of Dr. Burkitt's articles, published in the British Medical Journal, describes how populations living in developed countries strain to move fiber-deficient, small, hard and dry stools resulting in a much higher incidence of varicose veins, whereas there is little to no incidence in populations living in countries that consume diets rich in fiber, which produce soft, moist, bulky stools. Dr. Burkitt demonstrated that years of straining and bearing down to move difficult bowel movements creates tremendous retrograde pressures in the veins of the legs. This produces incompetent valves that are unable to hold up the weight of the blood resulting in sagging and bulging veins. High pressures dilate and stretch the values in the legs and can affect the elasticity in the vein walls as well. This is one reason why keeping our vascular system "young" and free from atherosclerotic buildup is so very important.
Doctor McDougall does a wonderful job at illustrating these points in the below video, Intestines From the Beginning.
Animal products and vegetable oils contain no fiber, while processed and refined foods have very little fiber. These foods promote disease and disability. However, a diet based on whole grains, beans, fruits, vegetables, and some nuts and seeds is loaded with fiber and promotes optimal health and wellness. If you'd like to learn more on the importance of a fiber-rich diet, and how it prevents and reverses other common Western diseases, see the blogs and articles below:
(1) Fiber's Many Unknown Benefits
(2) 97% of People are Deficient in This Nutrient
(3) Fiber Stops the Merry-Go-Round of Recirculation
(4) Fiber's Role in Preventing Breast Cancer
(5) Lower Your Cholesterol by Using Fiber!
(6) Straining for Relief – Damage Everywhere by John McDougall, MD
(7) Constipation, Hemorrhoids, Varicose Veins by John McDougall, MD
(8) The Benefits of Fiber by Dustin Rudolph, PharmD
(9) Is GERD a Symptom of Hiatal Hernia?
(10) What is Diverticulosis and What Causes it?
(11) Healthy Food = Healthy Colon
(12) Using Diet to Prevent Colon Polyps
(13) Dr. McDougall's Digestive Tune-Up (Book)
(14) Digestion Made Easy (DVD) by Michael Klaper, MD
(15) Denis Burkitt, MD Opened McDougall's Eyes to Diet and Disease
John McDougall MD Links
Preview the "Perfect Health Requires Perfect Circulation" Trailer
Blood Flow Boosts Vitality: Do factors that affect artery linings create or ease your aches and pains? Explore the link between impaired circulation and health challenges. How does blood flow relate to health troubles? Learn how Dr. Carney's science-based Starch-Smart® System can improve your circulation and overall health by nourishing endothelial cells at the start of your day.
When you subscribe to the blog, we will send you an e-mail when there are new updates on the site so you wouldn't miss them.