DrCarney.com Blog
What is Diverticulosis and What Causes it?
Diverticular disease is one of the most prevalent conditions in Western society which involves outpatient visits and hospitalizations. More than 100,000 Americans are hospitalized every year for this preventable condition. In some cases, a patient may develop life threatening complications such as a rupture of the intestines. As a hospital pharmacist, Dustin Rudolph PharmD sees many patients coming into the Emergency Room doubled over with abdominal pain. In his article, Diverticular Disease and Diet, Rudolph writes "This isn't your typical upset-stomach-because-you-ate-something-spicy kind of pain, but rather a severe give-me-morphine-now type pain."
What is Diverticular Disease?
Rudolph's article explains the difference between diverticulosis and diverticulitis: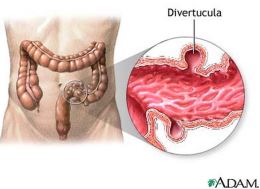
Diverticulosis – "Is the presence of one or several small, sac-like outpouchings, called diverticula, protruding from the wall of the colon. These diverticula are like little tiny pouches sticking out of the side of your colon."
Diverticulitis – "Is the acute inflammation of diverticula associated with fever, pain, and possible infections."
Rudolph clarifies that diverticulosis occurs first and that the majority of people aren't aware that they have it until it's discovered during a routine colonoscopy. Diverticulitis occurs when the diverticula become inflamed and is the reason why many come to the ER in pain. "Ten to twenty-five percent of affected individuals with diverticular disease will develop symptoms in the form of abdominal pain, bloating, irregular bowel movements, bleeding, or signs of infection." Out of these, "15% will develop significant complications."
What Causes Diverticular Disease?
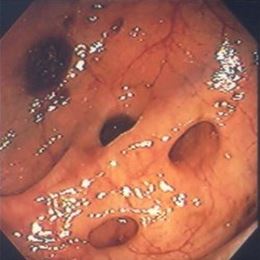 Multiple diverticula seen during colonoscopyDiverticular disease is not a consequence of genes or growing older. Diverticular disease is a result from years of eating a fiber-deficient diet. Diverticular disease was first noticed in the U.S. in the early 1900s; about the same time that processed foods began to be manufactured and introduced into the American diet. This greatly reduced fiber in the American diet.
Multiple diverticula seen during colonoscopyDiverticular disease is not a consequence of genes or growing older. Diverticular disease is a result from years of eating a fiber-deficient diet. Diverticular disease was first noticed in the U.S. in the early 1900s; about the same time that processed foods began to be manufactured and introduced into the American diet. This greatly reduced fiber in the American diet.
As digested food passes through the large intestine, water is absorbed, forming the stool. A diet lacking fiber from whole plant food stays in the colon longer due to low bulk weight resulting in a longer time frame for more water to be absorbed. The combination of little to no fiber and slow transit time in the colon produces stools that are small, dry, compact, hard, and low in bulk whereas stools produced from fibrous plant foods are large, moist and soft. Dr. Michael Greger explains that a "lifetime of straining to pass stools that aren't softened and bulked up by fiber can eventually balloon pockets out through the weakest points in the wall of our colons."
Diverticular Disease is a 20th Century Problem and a Disease of Western Civilization
When comparing the diets of populations living in developing countries to those living in industrialized Western countries, we see that the majority of calories in developing countries come from unrefined plant foods with the addition of small portions of animal and processed foods. The opposite is true for Western cultures. The majority of calories come from animal products and highly-refined processed foods. Diverticulosis is considered a 20th century problem and a disease of Western civilization. The highest rates of diverticular disease are seen in the United States and Europe; at least one person out of two over the age of 50 has diverticular disease with 60% of the population over the age of 60, and 80% in 80 year olds. On the other hand, those who eat a diet consisting primarily of whole plant foods have a 78% lower risk of developing diverticular disease. Yet this condition is nearly nonexistent in populations of people that consume high-fiber diets, such as in Japan or Africa, affecting less than 0.2% of the population. As countries become more industrialized they replace their native diets which are high in whole plant foods and low in animal products, with richer more Westernized foods which are low in whole plant foods and high in animal and processed food products. Thus, the rates of diverticular disease increase.
Meat and Processed Food Based Diets Promote Diverticular Disease
Meat–eaters have a much higher incidence of diverticular disease than vegetarians. Numerous studies show that consuming a diet centered on whole plant food is not only associated with a lower risk of hospital admissions and death from diverticular disease, but it also protects against developing it. In contrast, A large U.S. cohort study showed that "both a high red meat intake and low fiber intake (particularly a deficiency of fruit and vegetables) increased the risk of symptomatic diverticular disease by threefold. This finding was supported by a case-control study from Greece, where red meat was shown to increase the risk of symptomatic diverticular disease while vegetables and brown bread were protective." Other factors which could possibly complicate the condition are obesity, smoking, being sedentary, and the use of nonsteroidal anti-inflammatory drugs such as aspirin and steroids.
What is Fiber and Where is it Found?
 Fiber is found only in plant foods, including beans, whole grains and nuts/seeds. Animal products do not have any fiber.
Fiber is found only in plant foods, including beans, whole grains and nuts/seeds. Animal products do not have any fiber.
Just like bones form the frame of the human skeleton, fiber is the thread-like structure that forms the skeletal frame in plants. It's important to realize that only whole or minimally processed plant foods contain fiber, animal products do not. The typical American diet, which is rich in heavily processed foods, oils, animal products, and sugary drinks, is a fiber-deficient diet, since these products contain little or no fiber. Refined food contains very little fiber since the majority (if not all) is removed during processing. In contrast, a whole-food, plant-based diet supplies an abundance of fiber, more than twice the recommended minimum daily intake. Most Americans consuming the standard American diet eat a troubling 10-15 grams of fiber per day, whereas a plant-based diet can easily provide 60 to 100+ grams per day. In fact, 97% of Americans are deficient in this nutrient, especially those that consume high-protein (meat), low-carbohydrate diets.
There are two types of fiber in plant foods: soluble and insoluble. Soluble fiber dissolves in water and becomes a soft gel-like substance as it absorbs water. It becomes fermented by bacteria as it travels through the digestive tract. Insoluble fiber does not dissolve in water and passes through the digestive system nearly unchanged and has a laxative effect. Beans and other legumes are exceptionally high in fiber. Beans also contain a carbohydrate called "resistant starch" which has many of the same properties as fiber. As mentioned above, fiber provides the bulk (volume) of the stool. Those who eat a diet based on whole plant foods have large, soft stools that are passed effortlessly several times a day. Diets based on animal and processed foods however, produce very small, hard, marble shaped stool that takes great effort and force to pass. Rudolph says that "Fiber is essential to the formation of healthy bowel movements. Without it, or with very little of it, constipation can become a chronic problem leading to hard, compact stools requiring excessive straining to force out of the bowel." Dairy protein has also been shown to cause constipation, especially in children. Fiber not only keeps our gastrointestinal tract working optimally, it plays a much larger role in the prevention and reversal of disease. According to Dr. Michael Greger, "Stool size matters. The bigger our bowel movements, the healthier we may be." For additional information on fiber, see our Fiber Pinterest Board.
How Does Diverticular Disease Develop?
 Straining creates high pressure in the colonIn his article, Straining for Relief – Damage Everywhere, Dr. John McDougall explains in greater detail: "As the food moves through the small intestine the nutrients – protein, fats, carbohydrates, vitamins, and minerals – are absorbed through the intestinal wall into the bloodstream. Left behind are non-digestible matters (dietary fibers), colon bacteria and a few dead cells – these materials soon become the stool. Movement from the right side of the large intestine to the left side is accomplished by rhythmic contractions, known as peristalsis. In the final few inches of the large intestine, called the rectum, the feces accumulate. With adequate filling the rectum becomes distended, causing reflex contractions, which initiate the evacuation of the stool as a bowel movement. The remnants of digestion when consuming the Western diet produce only a small mass. These tiny rock-hard fecal marbles simply do not provide adequate filling to stimulate the rectum. Plus, because of their slow passage almost all of the water has been removed and they become dry and hard, thus more difficult to pass. To get them out requires enormous effort and harmful straining and therefore, high pressures. Years of elevated pressures [and straining to pass rock-hard stools] ruptures in the walls of the intestine, making balloons, called diverticula. Blood supply of the intestine begins on the outer surface, and then these small vessels dive through the muscular wall to supply the inner surfaces of the intestine. The weakest part of the wall of the intestine is where the blood vessels pass through the wall. As a result, the most common locations of these diverticula are next to blood vessels. Not surprisingly, one of the most common symptoms of this disease is bleeding. I have seen the bleeding so severe that the only way to save the person's life was to surgically remove the bleeding portion of the intestine. Picture a person seated on the toilet – grunting and groaning. The face is flushed red from blood pushed up into the head and neck. This is not the only direction blood is forced by straining. Blood diverted under pressure into all other body parts causes structural damage. After many years all this translates into diseases suffered by the majority of people living on the Western diet." Click here and here to view Dr. McDougall's video presentations on how diverticular disease develops.
Straining creates high pressure in the colonIn his article, Straining for Relief – Damage Everywhere, Dr. John McDougall explains in greater detail: "As the food moves through the small intestine the nutrients – protein, fats, carbohydrates, vitamins, and minerals – are absorbed through the intestinal wall into the bloodstream. Left behind are non-digestible matters (dietary fibers), colon bacteria and a few dead cells – these materials soon become the stool. Movement from the right side of the large intestine to the left side is accomplished by rhythmic contractions, known as peristalsis. In the final few inches of the large intestine, called the rectum, the feces accumulate. With adequate filling the rectum becomes distended, causing reflex contractions, which initiate the evacuation of the stool as a bowel movement. The remnants of digestion when consuming the Western diet produce only a small mass. These tiny rock-hard fecal marbles simply do not provide adequate filling to stimulate the rectum. Plus, because of their slow passage almost all of the water has been removed and they become dry and hard, thus more difficult to pass. To get them out requires enormous effort and harmful straining and therefore, high pressures. Years of elevated pressures [and straining to pass rock-hard stools] ruptures in the walls of the intestine, making balloons, called diverticula. Blood supply of the intestine begins on the outer surface, and then these small vessels dive through the muscular wall to supply the inner surfaces of the intestine. The weakest part of the wall of the intestine is where the blood vessels pass through the wall. As a result, the most common locations of these diverticula are next to blood vessels. Not surprisingly, one of the most common symptoms of this disease is bleeding. I have seen the bleeding so severe that the only way to save the person's life was to surgically remove the bleeding portion of the intestine. Picture a person seated on the toilet – grunting and groaning. The face is flushed red from blood pushed up into the head and neck. This is not the only direction blood is forced by straining. Blood diverted under pressure into all other body parts causes structural damage. After many years all this translates into diseases suffered by the majority of people living on the Western diet." Click here and here to view Dr. McDougall's video presentations on how diverticular disease develops.
What Causes Diverticulitis?
Diverticulitis occurs when these bulging outpouches (diverticula) become inflamed and infected. Dr. McDougall's article notes, "Diverticula become irritated by the unhealthy remnants of digested food in the large intestine, causing the openings to close, allowing the fluids to become stagnant and infected – a condition known as diverticulitis. In addition, the balance of the gut bacteria can also be altered due to chronic constipation and a low-fiber diet. Instead of a colon filled full of good (healthy) bacteria, there is an increase in bad (infectious-causing) bacteria that populate the colon. This can further increase the chances of an infection developing." Rudolph adds, "Constipation leads to stagnate fecal matter that finds itself sitting in the diverticula pouches. This in turn triggers inflammation of the intestinal wall. Pain, fever, bleeding, abscess formation (pus-filled sacs), and other complications can occur."
Should Nuts and Seeds be Avoided?
Many times during an autopsy, nuts, seeds or pieces of corn or popcorn are found in the diverticula pouches which led to the belief that these foods are what triggered the inflammation. Because of this, the majority of doctors advise their diverticular and elderly patients to avoid eating these foods. However, the lack of fiber in the diet is what caused the disease in the first place. Thus, cutting down on high-fiber foods not only promotes additional inflammation, it can lead to the formation of more diverticula. Rudolph explains that "Two studies have refuted this unfounded claim in recent years...nuts, corn, and popcorn consumption did not increase the risk of diverticulosis, diverticulitis, or diverticular bleeding." Dr. Michael Greger discusses this misconception in further detail here.
Prevention and Treatment Options
Eating a diet based on whole plant foods provides the fiber which forms the bulk of the stool. It also keeps the stool soft and moist making elimination quick, frequent, and painless. As a result from not having to exert tremendous strain and force, pressure is very low. Low pressure keeps the inside of the intestinal walls from ballooning outward, creating more diverticula. A plant-based diet also keeps existing diverticula from becoming inflamed and infected.
Dr. John McDougall says that a starch-based, high-fiber diet has relieved symptoms in 90% of cases of severe colon disease, including diverticular problems. "Patients with diverticular disease have much less trouble after they change to a healthy, high fiber, plant-based diet. A high fiber diet will also reduce the risk of future bleeding and infection and decrease the likelihood of developing new diverticuli." However, "the diverticuli that have already formed are permanent herniations of the colon, and will not disappear except by surgical removal, which is rarely indicated." Dr. McDougall also agrees that nuts/seeds don't get stuck in the diverticuli, causing inflammation.
Rudolph discusses several treatment options in his article. He emphasizes, "The best treatment for diverticular disease is prevention, but if you do happen to develop the condition there are a number of options to look at—the most important being a lifelong high-fiber diet consisting of unrefined, whole plant foods. The goal for any patient with diverticular disease is to not to have any recurrences of disease." Switching to a whole-food diet based on vegetables, fruits, whole grains and legumes is the best way to accomplish this. Rudolph explains the pros and cons of prescription drugs and antibiotics and their side effects here.
Click on the following for additional information:
(1) Dr.McDougall - Intestines from the beginning (Video)
(2) Dr. John McDougall Medical Message: Diverticulosis (Video)
(3) Diverticulosis: When our Most Common Gut Disorder Hardly Existed
(4) Dr. McDougall's Digestive Tune-Up (Book)
(5) Does Fiber Really Prevent Diverticulosis?
(6) Dr. Carney's "GI Disorders" Pinterest Board
(7) Dr. Carney's "Fiber" Pinterest Board
Scroll Down Page to Leave Comments

Want to Make Lifestyle Changes?
Not sure how to start? The good news is that Help is Only a Click Away! We invite you to join Dr. Carney's Helpful Sharing Community.
Preview the "Ask the Doc!" Trailer
Your Questions Answered: In Dr. Carney's Starch-Smart® System seminars, written questions from participants are collected beforehand, protecting their privacy. In this informative video presentation, Dr. Carney shares the answer to many of those frequently asked questions - with complex scientific evidence made easy to understand. Learn the answers to what you've always wanted to ask, and so much more!
When you subscribe to the blog, we will send you an e-mail when there are new updates on the site so you wouldn't miss them.